Gil-Vernet Sedo José María
- Our services
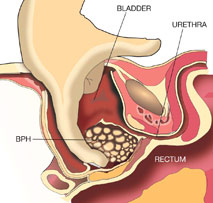 Surgical techniques are based on extraction, destruction or decreasing the size (atrophy) of BPH tissue to make a broad canal at the exit of the bladder, thus allowing urination without problems. These techniques do not eliminate all of the prostate gland, as its removal is only indicated in patients with prostate cancer.
Surgical techniques are based on extraction, destruction or decreasing the size (atrophy) of BPH tissue to make a broad canal at the exit of the bladder, thus allowing urination without problems. These techniques do not eliminate all of the prostate gland, as its removal is only indicated in patients with prostate cancer.
Open prostatectomy. This was the first procedure to be used (practiced since the end of the 19th Century) and it is currently recommended for very large prostates (> 90 grams) with or without the presence of large stones, bladder diverticula, urethral stenosis (tightening of the urethra) or concomitant inguinal hernia.
The procedure is carried out under general or regional (spinal) anesthesia. The surgeon makes a small incision between the belly button and the pubic bone. The prostate is reached through the bladder or the bladder neck, and all of the BPH tissue is removed. A urethral catheter is placed that is removed five days after the procedure. The hospital stay ranges from 5 to 7 days. In most cases the outcome is excellent and the patient has increased urinary flow compared to other less invasive procedures (TUR or laser), and there is minimal incidence of repeat intervention or urethral stenosis (tightening). With current surgical techniques, blood transfusion is only necessary for 7% of patients.
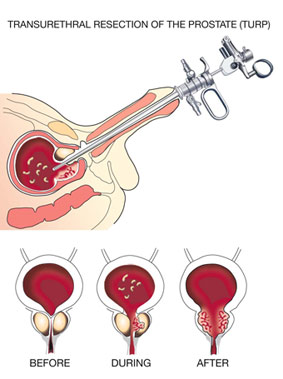 Transurethral resection (TUR) of the prostate. This technique was first described in the 1920's and its use spread extensively in 1970. Since then, the gradual implementation of new technologies has introduced improvements in this technique. Currently TUR of the prostate is considered to be the most effective surgery for treatment of BPH. It is estimated that 95% of surgeries for prostates between 30 and 90 grams utilize this technique. To demonstrate the efficacy of the most innovative procedures, such as laser techniques, they are compared against TUR.
Transurethral resection (TUR) of the prostate. This technique was first described in the 1920's and its use spread extensively in 1970. Since then, the gradual implementation of new technologies has introduced improvements in this technique. Currently TUR of the prostate is considered to be the most effective surgery for treatment of BPH. It is estimated that 95% of surgeries for prostates between 30 and 90 grams utilize this technique. To demonstrate the efficacy of the most innovative procedures, such as laser techniques, they are compared against TUR.
The operation is carried out under general or regional (spinal) anesthesia with a resectoscope, an instrument inserted into the urethra that uses an electrical current to cut the BPH tissue into fine slivers and clot any points of bleeding. Due to the use of irrigation liquids, the surgery should not last more than 2 hours due to the risk of changes in the ion concentration of the blood (hyponatremia). The hospital stay ranges between 2 and 3 days.
Plasmakinetic TUR and prostate vaporization.
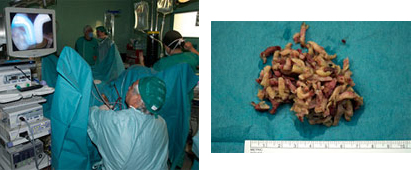 This is the most advanced TUR technique in which electrical energy converts the saline solution into a plasma cloud with a field of ionized particles that permit a precise "cut and seal," cutting the length of the procedure in half compared to classical TUR. Other advantages of bipolar TUR (plasmakinetic system) include the possibility of treating prostates of greater size with minimal blood loss and with a much shorter post-operative period with fewer problems. This technique also allows for a vaporization system that effectively destroys the prostate tissue. The hospital stay is 1 or 2 days.
This is the most advanced TUR technique in which electrical energy converts the saline solution into a plasma cloud with a field of ionized particles that permit a precise "cut and seal," cutting the length of the procedure in half compared to classical TUR. Other advantages of bipolar TUR (plasmakinetic system) include the possibility of treating prostates of greater size with minimal blood loss and with a much shorter post-operative period with fewer problems. This technique also allows for a vaporization system that effectively destroys the prostate tissue. The hospital stay is 1 or 2 days.
| Morning | Afternoon | |
|---|---|---|
| Monday | 10.00 - 14.00 h | 16.00 - 19.00 h |
| Tuesday | 10.00 - 14.00 h | 16.00 - 19.00 h |
| Wednesday | 10.00 - 14.00 h | 16.00 - 19.00 h |
| Thursday | 10.00 - 14.00 h | 16.00 - 19.00 h |
| Friday | 10.00 - 14.00 h | - |















