Riambau Alonso Vicente
What is an aneurysm?
An aneurysm is an abnormal narrowing of an artery, normally caused by arteriosclerosis (degenerative hardening of the arteries), hypertension or chronic infections. The majority of aortic aneurysms are asymptomatic. An aneurysm may appear in any artery of the human body, but it more frequently occurs in the aorta, especially at the level of the kidneys and the larger arteries of the legs (abdominal aortic aneurysm).

Abdominal Aortic Aneurysm in Scanner 3D (MMS®)
- What are the risk factors?
- Older than 60 years of age
- Male
- Smoker
- Family history of aneurysms
- Arterial hypertension
- Chronic bronchitis
- What symptoms does it cause?
Initially, aneurysms do not engender symptoms. Unfortunately, they usually appear, as a complication or a rupture. Both in abdominal and thoracic aortas, the rupture produces a block of hypovolemic shock, that is to say, a loss of consciousness from internal hemorrhaging. Sometimes, a sensation of intense abdominal or thoracic pain precedes this symptom, according to the site of the aneurysm. The prognosis is very grave and the patient should be rushed to a hospital emergency room.
In thin patients, by palpating the abdomen, an aortic aneurysm can be detected. Sometimes, thoracic aneurysms affect the recurrent nerve, giving rise to a loss or alteration of voice of an apparently unjustified cause.
For this reason, the diagnosis of aortic aneurysms is of a fortuitous nature. That is to say, they are often found during the course of an examination by palpating the abdomen or by examining the abdomen by sonogram, CT or MRI or because of medical reasons. Frequently, CT of the thorax of the vertebral column discovers thoracic aneurysms.
- What is the Treatment?
If the aneurysm is small, with unlikely probability of rupture or complications and is located within the abdominal aorta, its progression can be followed by regular sonography. If it is of a larger size, expanding or its location is precarious, treatment consists of substituting the aneurysmal portion of the artery with an artificial artery of synthetic material. For this purpose, the conventional surgical technique employs large incisions to reach the area of the aorta, clamp it and replace the aneurysm with a synthetic vascular graft by sewing it to the healthiest vascular extremes. This technique which we have been performing for dozens of years, is being progressively replaced by endovascular techniques which offer similar results by means of less aggressive procedures.
The new endovascular techniques, permit, when the anatomy is favorable, to treat the aneurysm by means of placing an expandable graft, inside the vessel, without the necessity of open surgical procedures (by means of the vessels of the extremities, commonly the femoral arteries). The graft is introduced by means of catheterization and is spread out in a determined position guided by fluoroscopy of high definition. Blood circulates inside the graft and, likewise, is protected from growth and rupture of the aorta, leading to a reduction in size with time.
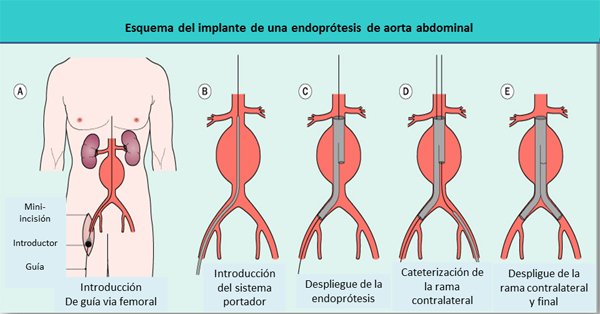
Scheme of implantation of a graft of the abdominal aorta
- Mini-incisions
- Introducer
- Guide
- Introduction of the guide by the femoral artery
- Introduction of the carrier system
- Unfolding of the graft
- Characterization of the contralateral branch
- Spreading out of the contralateral branch and digit
- What is endovascular surgery?
In the last decade, we medical professionals have been aiding in an inevitable technological progress by applying imaging and therapeutics processes to the methods of diagnosis. This has resulted in an increase in numerous minimally invasive techniques as an alternative to more conventional surgical procedures. Vascular pathology has not escaped this majority trend. Perhaps the pathology of the aorta can potentially benefit more clearly from these new approaches, now that the margin of benefits in terms of reducing morbidity and mortality is greater. But how does one define endovascular treatment?
It is that therapeutic act, which by employing a more remote point of entry, whether it be percutaneous or by means of dissection, by applying means of catheterization is able to repair a further vascular segment, by generally using fluoroscopic vision (or radioscopic) as a method of control.
- Since when has endovascular surgery been performed and what is the existing experience?
From the first clinical experience in the endovascular repair of abdominal aortic aneurysms in 1990, more than 300,000 synthetic grafts have been placed in abdominal aortic aneurysms and more than 30,000 commercially made grafts in thoracic aneurysms (some 5,000 and 1,000, respectively, in Spain).
- What specialists take part in endovascular surgery?
In the therapeutic process, several professionals participate, from the diagnosis, selection of the patients and the appropriate procedures and post-operative therapeutic follow-up. All of these are equally important in order to ensure the technical and clinical success and should be applied with equal interest, dedication and professionalism.
In particular, in our center, in the multidisciplinary team of endovascular therapeutics of the aorta, the vascular surgeon (leader and responsible one of the team), cardiovascular anesthesiologist, interventional vascular radiologist, expert in transesophageal CT´s), radiologist expert in vascular imaging (CT and MRI), cardiovascular surgical nurse, interventional vascular radiology technicians, participate. All of these unswervingly dedicated professionals participate in the different processes that endovascular treatment of the aorta entails.
The teams must have the demonstrated skill in endovascular treatment as well as in conventional surgery.
- For what pathologies is endovascular treatment indicated?
If we focus on the pathology of the aorta, concretely aortic and thoracic aneurysms, 5 - 10% of male patients older than 65, suffer from these, which pose an implicit threat to their lives. We understand that any solution or improvement in their diagnosis, and especially in their treatment, involves all the professionals that deal direct- or indirectly with this pathology and evidently for the patients that suffer from it. It is in the repair of the aortic and thoracic aneurysms in which this technique has its greatest and most prominent application.
Pathologies such as the acute aortic syndrome (acute type B dissection, penetrating ulcers, intramural hematomas) traumatic injuries, pseudoaneurysms, chronic type B dissections, and aortobronchial and aorto-esophageal fistulas are potentially treated by means of an endovascular technique. Because of this, endovascular treatment of thoracic aneurysms merits special consideration both for patients, as well as for health care professionals.
Other grave vascular pathologies such as severe ischemia of the lower extremities or obstructions of the cervical or carotid arteries are potential indications for endovascular techniques.
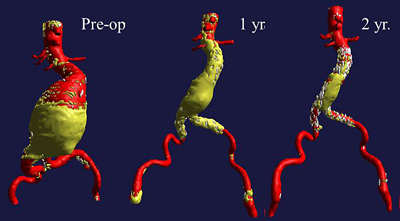 Before Endovascular Treatment,at one year and at two years, when the aneurysm has disappeared.
Before Endovascular Treatment,at one year and at two years, when the aneurysm has disappeared. - Indications for Abdominal Aortic graft
The selection of patients for the endovascular treatment of an abdominal aortic aneurysm requires more time and more commitment than for conventional open surgery. The technique was initially conceived for high-risk surgical patients who have an abdominal aortic aneurysm considered to be surgical by its dimensions (more than 5 cm in diameter), with rapid growth (more than 0.5 cm in six months) or symptomatic aorta (embolization, pain…) Likewise, these patients should not have any medical conditions that might suggest a life span less than two years), nor accompanying septic processes, nor allergies to metallic components of the graft. In addition, some indispensable anatomic or morphometric requisites should come together in order to anchor with certainty the femoral arteries, not occluding essential branches of the abdominal or iliac arteries (renal or hypogastric arteries), and accessing from the femoral arteries. In exceptional cases, the graft and special techniques for complex anatomies to which few equipment has access, may be used. Our team is authorized and counts on broad experience in the treatment of complex aortic aneurysms.
Currently this procedure is accepted for patients of normal risk, whenever the patient has a favorable anatomy, has received reliable information about the ultimate risks of the technique and its traditional alternative, and of the therapeutic team, and agrees to do the necessary follow-up. Besides, the procedure by expert teams (more than 40 procedures and more than 20 per year) and the selected graft should be the most adaptable one and that has demonstrated the best long-term results.
- Results of the Abdominal Aortic grafts
In the Eurostar series, with more than 10,000 cases included, the immediate mortality recorded within the first 30 days after surgery is less than 2%, 5% of which are directly related to the procedure. The remaining registered deaths correspond to myocardial infarctions, respiratory failure, multi-organ system failure or sepsis. The mortality is greater in those patients considered not candidates for conventional or general anesthesia. Both the general conditions of the patient as well as the necessity of applying adjuvant therapies during the procedure are related significantly to the greater numbers of immediate mortality. The cumulative survival at five years of follow-up is around 77.2%. In our group, the perioperative mortality is around 1% and the survival rate at five years is 82%.
Conventional surgery offers a perioperative rate around 4% and a rate of complications around 20%. International multi-centric prospective studies that compare open surgery with endovascular, coincide, emphasizing that endovascular treatment results in a drastic reduction of mortality and complications related to surgery, length of hospital stay in the ICU and medical units, the need for transfusion and recovery time of the patients.
Principal complications: endoleaks (any presence of circulating blood in the aneurysmal sac, between the graft and the wall of the aorta), constitute the principal complication. The rate of leaks in our group is 6%, the majority of them without clinical repercussions and with favorable outcomes.
Of the data corresponding to the afore-mentioned studies, it follows as a logical corollary that the lesions in the access point are calculated to be 4%. Approximately 1% of the cases are not complicated because of difficulty with their access. The association with adjuvant processes and the lack of experience of the therapeutic team constitute clear risk factors for vascular complications and the necessity of aborting the procedure. Conversion to emergency open surgery are in 1% of the cases, augmenting the mortality of the procedure up until 15%.
In our experience of about 20 years, with more than 1,300 endovascular cases of the aorta performed, the rate of conversion to open surgeries is 0%, the overall rate of complications does not reach 3% and the rate of mortality is less than 1%.
Throughout the procedure, other possible complications may occur, the worst and most likely are secondary endoleaks, migrations, infolding and the rupture of the potentially treated AAA. All of these can lead to the need to perform an endovascular re-intervention or open surgery. In our experience, we have not needed to convert any patient to open surgery, with the rate of re-intervention less than 6%. In our series, the average hospital stay has been less than two days.
In general, and as an example, an endovascular repair of the third portion of the descending thoracic aorta can be performed under local anesthesia, with a surgical time of less than one hour, without consumption of blood products nor special facilities, with a hospital stay of less than two days and an almost immediate physical recovery of the patient. Nevertheless, the uncertainty of the durability of this method is an argument which some critics of the technique put forth. For the majority, the technology on which endovascular treatment is based is solid and with time’s demonstrating its enormous utility, owing to the favorable experience of the cases treated.
Just as it occurs for the abdominal endografts, patients must meet the anatomical and morphological requisites in order for the endograft to be securely anchored, without occluding indispensable branches of the thoracic aorta (or coronary, supra-aortic, visceral or spinal arterial trunks, as well as access from the femoral arteries.
- Indications for Thoracic Aortic Endograft
When dealing with the conventional factors of high-risk surgery, the endovascular technique enjoys greater use in the thoracic sector for patients with better general conditions than in the abdominal sector. In other words, when the surgical risk in relation to surgical repair is greater than what is reasonably acceptable, at the present time, endovascular repair is preferable, above all in medical centers with experience in performing it. Additionally, the favorable cost/benefit relationship with these types of pathologies, given that the endograft offers a less aggressive alternative and more effective, in short to medium terms, because, additionally results in being more economical than traditional surgical methods.
In general, and as an example, an endovascular repair of the third portion of the descending thoracic aorta can be performed under local anesthesia, with a surgical time of less than one hour, without administering blood products, or requiring special facilities, with a hospital stay of less than two days and an almost immediate recovery of the patient. Nevetheless, the uncertainty of the durability of this method is an argument which some critics of the technique propose. For the majority, the technology on which endovascular treatment is based, is solid and with time´s demonstrating its enormous utility, owing to the favorable experience of the cases treated.
Just as it occurs with the abdominal endografts, patients must meet the anatomical and morphological requisites in order to be able to anchor with certainty the endograft, without occluding indispensable branches of the thoracic aorta (or coronary, supra-aortic, visceral or spinal arterial trunks), as well as gaining access from the femoral arteries.
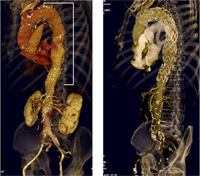 Images of a large aortic-thoracic aneurysm. At the right, a control at five years of repair of the descending thoracic aortic with endograft without complications.
Images of a large aortic-thoracic aneurysm. At the right, a control at five years of repair of the descending thoracic aortic with endograft without complications.
| Morning | Afternoon | |
|---|---|---|
| Monday | 09.00 - 21.00 h | - |
| Tuesday | 09.00 - 21.00 h | - |
| Wednesday | 09.00 - 21.00 h | - |
| Thursday | 09.00 - 21.00 h | - |
| Friday | 09.00 - 21.00 h | - |















