Dr. Aleix Vida'ls team
Anatomy of the knee
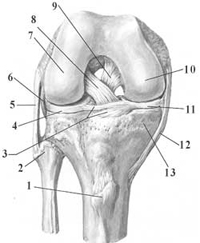
The knee joint is formed by the distal femur, proximal tibia and the patella. There are ligament structures that provide stability to the bones: collateral ligaments and cruciate ligaments.
The entire surface of the knee is covered with a smooth structure called articular cartilage which allows a smooth gliding motion. Inside the knee joint there are two semicircular rings of cartilage called "menisci" that act as cushions. The synovial fluid is the lubricate that reduces joint friction.
- Meniscus Injury
The menisci can be damaged by playing sports or during daily activity due to repeated impact or twisting of the knee. Meniscal tears cause pain, swelling, weakness and giving way.
Treatment of the torn meniscus may be: arthroscopic repair of the tear or resection of the damaged meniscus leaving the remaining healthy meniscus intact.
Knee arthroscopy is performed under out-patient basis. The patient can walk home with crutches. Recovery is complete in 90-95% of cases within 4-6 weeks. If there are other injuries associated with the meniscal damage recovery may be prolonged up to three months.
 Meniscal tear and repair of the meniscus
Meniscal tear and repair of the meniscus - ACL Injury
The cruciate ligaments (anterior and posterior) act as stabilizers of the knee. Injury to the anterior cruciate ligament (ACL) is the most common and usually occurs when making a sharp turn on the knee in sports such as skiing or soccer. When you are injured there is pain, swelling and difficulty walking.
We tend to recommend non-operative treatment for ACL injuries in cases of partial or complete tears when the knee maintains acceptable stability. A specific rehabilitation program is advised to avoid twisting motion of the knee.
For unstable knees with associated meniscal injury or in patients performing high-demand sports surgical treatment is advised. Reconstruction is done by creating a new ligament from a knee tendon. The tendon can be from the patient's own knee (autograft) or from a donor (allograft). Patients can walk immediately with the aid of a brace and crutches. The surgery is effective in 85% of cases, being able to return to the practice of sport at 4-6 months after surgery.
 Cruciate ligament rupture and reconstruction with tendon graft
Cruciate ligament rupture and reconstruction with tendon graft - Posterior cruciate ligament injury
The lesion of the posterior cruciate ligament (PCL) is frequently related to traffic accidents or when performing a sport. The ligament may be injured in isolation or associated with other injuries of the meniscus and other ligaments resulting in pain, swelling and difficulty walking impairment.
Conservative treatment is recommended when the knee maintains stability that means the knee joint moves with its normal congruity. Treatment consists of a rehabilitation program and re-educational therapy.
When we have unstable knees due to ligament injuries surgical treatment is advised. Reconstruction is accomplished by creating a new ligament from a knee tendon. The tendon can be patient's knee (autograft) or from a donor (allograft). Tunnels are drilled through the bone to insert and fix the graft. In the post-opertaive period patients can walk with the aid of a brace and crutches. Rehabilitation continues for a few months.
 Guiding during posterior cruciate ligament reconstruction
Guiding during posterior cruciate ligament reconstruction - Articular cartilage injury
The entire surface of the knee is covered with a chodral layer called cartilage which allows a smooth gliding motion. During sports or normal daily activity cartilage injuries can occur, isolated or associated with other injuries. Symptoms occurring after cartilage injuries are pain, swelling, locking and weakness.
The treatment of these lesions consists with arthroscopic repair. Small lesions are usually treated with arthroscopic polishing or by performing micro-perforations that cause scar tissue to cover the lesion. In more severe injuries the treatment consists of osteochondral grafting from the same knee chondrocytes transplant harvested from the patient.
The recovery process is long (months) and the final result depends crucially on the extent and size of the lesion, patient age and activity level. Large cartilage lesions can lead to early osteoarthritis of the knee.
 Healthy cartilage and injured cartilage
Healthy cartilage and injured cartilage - Patellar problems
The patella is the small bone that we palpate in front of the knee. It slides in the femoral groove with flexion and extension. It is covered with a chondral surface called cartilage allowing a smooth sliding movement.
Patello-femural problems are usually related to the patella cartilage degeneration (chondromalacia)or patello-femural instability (dislocations). The main complaints are pain, (mostly while walking down stairs) swelling and giving way.
Initial treatment is conservative and consists of rehabilitation, medication and orthotics (braces). If conservative treatment fails, surgical treatment is advised. It consists arthroscopic examination, smoothening of articular cartilage and patellar release or realignment to allow proper gliding.
 Healthy cartilage and injured cartilage
Healthy cartilage and injured cartilage - Knee Osteoarthritis
Knee Osteoarthritis is characterized by the deterioration and the loss of articular cartilage and inflammation. The patient has pain mainly at night, swelling and difficulty walking.
Initial treatment is conservative: medication and physical therapy. In intermediate stages without serious joint deterioration, we perform infiltration of hyaluronic acid or with PRP (growth factors). Arthroscopy can help maintain joint function and control pain and good results are obtained in knees with no major deformities or advanced joint disease. The surgery is performed under out-patient protocol. The patient can walk away with crutches. This is a treatment that can alleviate the discomfort an indeterminate time period.
In advanced stages of osteoarthritis associated with severe articular damage knee replacement is the solution.
 Image before and after knee arthroscopy in osteoarthritis
Image before and after knee arthroscopy in osteoarthritis - Fractures of the Knee
The practice of certain impact sports (skiing, soccer, basketball) can cause fractures around the knee. The main symptom is pain associated with swelling. The most common fractures are the ones that involve the tibial plateau: tibial eminence avulsion fracture (TEAF) and osteochondral fractures are frequently seen sport trauma.
When the fracture is displaced, surgical treatment indicated. Routine surgical methods include open surgery that can end in a large scar and painful postoperative period. Better cosmetic outcome and a more comfortable postoperative period is achieve through arthroscopy as well as less joint damage thus allowing better recovery.
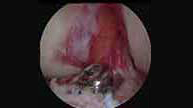
Arthroscopic view of fracture repair and screw fixation
| Morning | Afternoon | |
|---|---|---|
| Monday | 08.00 - 20.00 h | - |
| Tuesday | 08.00 - 20.00 h | - |
| Wednesday | 08.00 - 20.00 h | - |
| Thursday | 08.00 - 20.00 h | - |
| Friday | 08.00 - 15.00 h | - |















