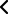

Enfermedades de Glándula Mamaria
 Hay pocos motivos de mayor preocupación o de alarma que encontrarse un "bulto" o tumor en la mama. Siempre se piensa lo peor y más dramático. Las reacciones son diferentes y bien distintas, desde las personas que consultan rápido al médico, a personas con miedo a comentarlo a nadie y que por tanto demoran el diagnóstico y las posibles soluciones.
Hay pocos motivos de mayor preocupación o de alarma que encontrarse un "bulto" o tumor en la mama. Siempre se piensa lo peor y más dramático. Las reacciones son diferentes y bien distintas, desde las personas que consultan rápido al médico, a personas con miedo a comentarlo a nadie y que por tanto demoran el diagnóstico y las posibles soluciones.
Es normal que una persona se siente angustiada y preocupada por presentar un "bulto" en la mama, en principio lo antes que lo note y lo pequeño que sea, más posibilidades de curación tendra si es cancer. No todos los "bultomas"son malignos, se debe consultar a un profesional para que pueda diagnosticarlo de manera correcta y si procede realizar el tratamiento adecuado.
No nos podemos olvidar que el cancer de mama es el más frecuente en las mujeres y es la segunda causa de mortalidad de las mujeres con cancer, después del cancer de pulmón pero también hay que constatar que si el tumor es pequeño y no hay ganglios el índice de supervivencia es superior al 95 % . La mamografía sigue siendo la prueba de elección.
- Generalidades y exploraciones
El borde mamario o línea de los pezones aparece en la sexta semana del desarrollo del embrión y se identifica en la forma de un engrosamiento ectodérmico desde la axila hasta la ingle. Los dos tercios caudales de dicha línea muestran regresión y su persistencia anómala a menudo se confunde con nevus o lunares. El tejido mamario aberrante en la axila o en cualquier punto fuera del borde mencionado se manifiesta durante la estimulación hormonal propia del embarazo y su tratamiento es extirpación quirúrgica.
La disminución de los niveles de estrógeno de la madre después del nacimiento estimula la producción de prolactina por el neonato con secreción de calostro (leche de brujas) durante varios días en niños y niñas.
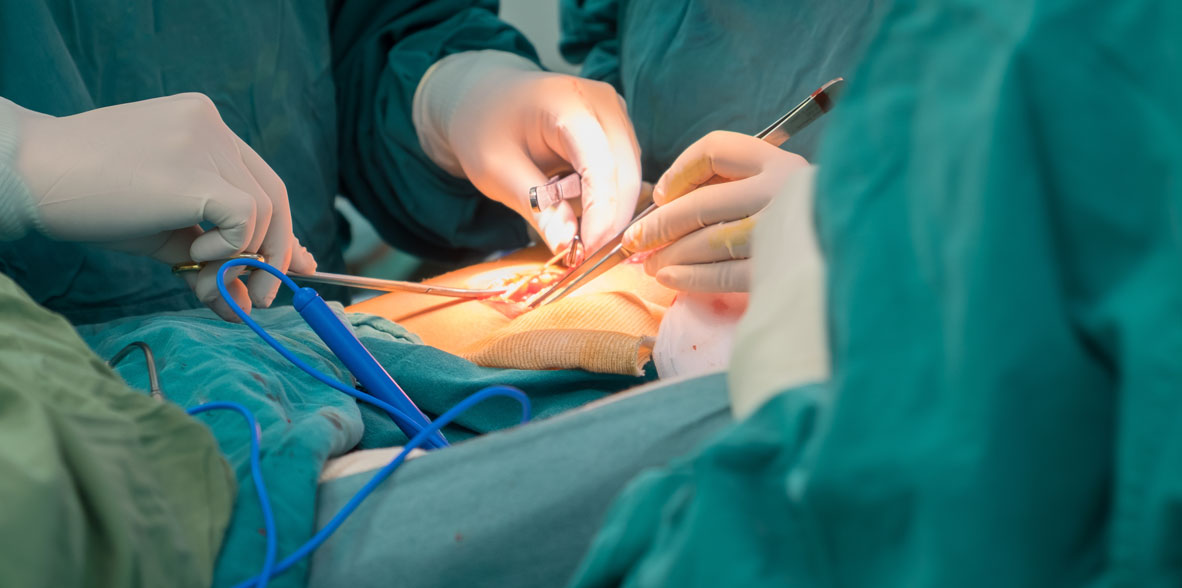
Excepto la hipertrofia leve durante el periodo neonatal y la pubertad, la zona mamaria del varón muestra pocos cambios durante toda la vida. El "montículo" prepuberal de la mujer surge entre los 11 y 15 años. Hay formación de lóbulos después de la primera ovulación. El seno de la joven adulta se extiende de la segunda a la sexta costillas y desde el esternón a la línea axilar anterior. E1 tejido glandular tiene una forma circular, excepto la cola de Spence, que llega a la axila. Los ligamentos fibrosos de Cooper suspenden el tejido glandular de la aponeurosis superficial anterior debajo de la piel. El área subareolar y el pezón contienen músculo liso que se contrae con la estimulación táctil.
Los ganglios linfáticos del área de la mamaria interna y axilar se encargan del drenaje del seno.
Niveles axilares: I, por fuera del pectoral menor; II, por debajo del pectoral menor; III, por dentro del pectoral menor. Los ganglios de Rotter constituyen un grupo que se localiza entre los músculos pectoral mayor y menor. El drenaje se hace de abajo hacia arriba y al final a ganglios supraclaviculares, y después por el conducto torácico al sistema venoso. El número promedio de ganglios linfáticos registrado en operaciones es de cinco ganglios mamarios internos y 20 ganglios axilares (niveles I, II y III).
Fisiología
El desarrollo y función de la mama se inicia por diversas hormonas. Se sabe que el estrógeno estimula la formación de los conductos mamarios. La progesterona comienza el desarrollo de los lobulillos de la mama y la diferenciación de células epiteliales. La prolactina estimula la lactogénesis. Cambios cíclicos: el volumen aumenta casi 50% después del octavo día del ciclo menstrual. La congestión vascular y la proliferación lobulillar muestran regresión con la menstruación.
- Embarazo y lactación: los conductos alveolares lobulillares proliferan después de la regresión que acontece al cesar la fase de amamantamiento. Se oscurecen el pezón y la areola y sobresalen las glándulas de Montgomery de la areola. Aparecenestrías.
- Menopausia: los lobulillos involucionan y la grasa sustituye al parénquima.
- Aberraciones: el desarrollo asimétrico o la hipertrofia virginal en jovencitas pueden corregirse quirúrgicamente después de la madurez. La ginecomastia en varones púberes se corrige si no hay reversión ni anormalidades hormonales.
Exploración física
- Inspección: el operador puede detectar más fácilmente asimetría, depresiones cutáneas, edema e inversión del pezón si la mujer esta sentada, con las manos sobre la cadera y después las eleva por arriba de la cabeza.
- Palpación: con la paciente sentada y luego erecta, el operador explora la zona supraclavicular y la fosa axilar, y también la cola de Spence y el tejido mamario central. Se vuelve a revisar todo el seno con la mujer acostada sobre su espalda y con los brazos por encima de la cabeza. Son características importantes de un tumor o ganglio su tamaño, forma, movilidad y fijación.
- Estudios:
- Mamografía: La American Cancer Society recomienda mamografías "básales" entre los 35 y 40 años, después cada dos años entre los 40 y 50 años, y cada año después de los 50. Si existen antecedentes familiares hay que obtener el primer mamograma a los 35 años y una placa anual después de los 40. El mamograma valora los cambios del estroma, en contraste con las áreas grasas del seno, de modo que es más preciso en los senos grasos de posmenopáusicas que en los senos glandulares de las premenopáusicas. Los patrones sospechosos de carcinoma incluyen engrosamiento de la piel, densidades del estroma con invasión "radiada" del parénquima y microcalcificaciones (restos expulsados al interior de los conductos por células de división rápida, especialmente común en cánceres intracanaliculares). La mamografía es especialmente útil en la exploración de lesiones no palpables, para estudiar el seno contralateral en mujeres con cáncer, y en el seguimiento de la mama ipsolateral después de un tratamiento conservador de Cancer. La frecuencia de resultados falsos positivos es de 11% y la de falsos negativos 6%. Los estudios prospectivos demostraron detección mas temprana del cáncer y mayor supervivencia gracias a la identificación por mamografía. La Xerorradiografía es semejante a la mamografía pero de imágenes positivas en vez de negativas y aumenta la exposición a la radiación, razón por la cual no se recomienda. Termografía: los tumores o infecciones generan "zonas calientes", pero constituyen un método poco fiable.
- Ultrasonografía: los quistes se distinguen de las lesiones sólidas por medio del ultrasonido, pero con este método no se detectan microcalcificaciones. La aspiración con aguja es una técnica mas sencilla y menos cara para detectar quistes. Su principal indicación consiste en estudiar lesiones sospechosas no palpables en la mamografía.
- Otros métodos: la tomografía por computadora y la resonancia magnética nuclear aún están en fase experimental en la detección de cáncer mamario.
- Ductografía: consiste en la inyección de contraste radiopaco en un conducto galactóforo. Se indica ante secreciones por el pezón, en particular si son sanguinolentos.
- Patología benigna mama
Mastopatía fibroquística
Llamada de muchas maneras, entre otras mastitis quística crónica, este trastorno aumenta en incidencia con la edad, pero tiende a generar mas síntomas en mujeres jóvenes, y antes de la menstruación también se advierte dolor e hinchazón de los senos. Unicamente las mujeres con hiperplasia intensa o atipia en la biopsia están expuestas a mayor riesgo de carcinoma. Nunca se han corroborado las afirmaciones de alivio sintomático con la ingestión de vitamina E o la abstinencia de cafeína o derivados xantínicos.
Se han utilizado eficazmente en el tratamiento Danazol (análogo androgénico sintético), tamoxifeno (un antiestrógeno) e incluso la progesterona.
Quistes
Estas masas circunscritas, firmes y redondas varían de 1 mm a varios centímetros de diámetro y pueden aumentar su tamaño alfinal del ciclo menstrual. En la aspiración, en forma típica, el líquido es transparente o verde pardusco y no requiere examen citológico. La biopsia está indicada si el líquido es sanguinolento, si la masa no muestra resolución completa después de la aspiración, o si se acumula el líquido mencionado.
Fibroadenomas
Estas masas lobulillares, firmes, coriáceas y circunscritas suelen ser solitarias y aparecer en mujeres jóvenes; se tratan mejor por ablación en mujeres mayores de 25 años. En las pacientes más jóvenes, conviene limitarse a efectuar estudios citológicos poraspiración con aguja y mantenerlas bajo vigilancia.
Papiloma canalicular
En promedio, 33% de las mujeres con secreción sanguinolenta por el pezón tienen un papiloma intracanalicular, a pesar de que casi 20% tienen carcinoma. El diagnóstico se confirma por ductografía. La ablación del sistema de conductos principales y tejido mamario en el área subareolar se practica con la ayuda de una sonda lagrimal como guía, que se introduce dentro del conducto que secreta.
Otras lesiones
- Adenosis esclerosante: áreas fibróticas irregulares de tejido mamario con microcalcificaciones, que necesitan biopsia para diferenciarlas del carcinoma.
- Necrosis grasa: en promedio, solamente 50% de las mujeres con necrosis grasa recuerdan el traumatismo relacionado con ella, que ocasiona áreas de fibrosis intersticial, firme e irregular con retracción de la piel a menudo se confunde con carcinoma, hasta que se hace el estudio histopatológico Mioblastoma de células granulosas de la mama, de aspecto macroscópico semejante al cáncer mamario incipiente.
- Enfermedad de Mondor, que es la tromboflebitis de una vena superficial del seno, a menudo con dolor y retracción de la piel.
- Las infecciones agudas son más comunes en mujeres que amamantan y que sufren abrasiones del pezón, y a menudo se acompañan de dolor y eritema. La celulitis puede tratarse con antibióticos, pero los abscesos requieren incisión, corte de las loculaciones y drenaje en declive (por lo común se identifica en el cultivo Staphylococcus aureus). Las mujeres que no amamantan necesitan biopsia y drenaje para diferenciar entre ectasia de conductos y abscesos que son secundarios a la obstrucción ausada por el carcinoma canalicular.
- La infección crónica es rara, excepto en pacientes inmunosuprimidas, pero desde el punto de vista histológico suele ser causada por tuberculosis, que proviene de los pulmones o de la erosión de un cartílago costal por parte de un ganglio mediastínico.
Enfermedades de Glándula Mamaria: carcicoma
El carcinoma mamario es el cáncer más común en mujeres en Estados Unidos, y desde 1940 ha aumentado la incidencia ajustada a la edad; actualmente se le diagnostica en una de cada nueve estadounidenses durante su vida. La tasa de mortalidad por cáncer de mama sólo se ubica por detrás del cáncer pulmonar.
Es probable que su causa sea multifactorial. El sexo femenino constituye un factor predisponente, dado que sólo un varón muestra carcinoma mamario por cada 100 mujeres diagnosticadas.
La incidencia aumenta con la edad. Comienza después de los 20 anos y alcanza un nivel estable (meseta) alrededor de la menopausia, para después aumentar en forma neta a continuación de ese cambio. Los factores genéticos son importantes en 15% de los casos, y son más notables en mujeres cuya madre tuvo carcinoma en ambos senos antes de la menopausia. Inglaterra y Gales tienen la mortalidad nacional por cáncer de mama más alta y Japón la más baja.
El riesgo mayor guarda relación con nuliparidad y con el primer embarazo en los últimos años de fertilidad. Los estrógenos inducen el cáncer mamario en ratones, pero en los seres humanos no se ha corroborado ninguna teoría de inducción por hormonas o píldoras anticonceptivas.
Entre los factores de riesgo que se han propuesto están obesidad, consumo abundante de grasas animales y factores vírales transmitidos por la leche materna.
El curso natural de la enfermedad se ha citado en estudios desde finales del siglo pasado, en el Hospital Middlesex, de Londres, en que la mediana de supervivencia en 250 mujeres no tratadas fue de 2.7 años; la supervivencia se calculó con base en la descripción del comienzo de los primeros síntoma.
La supervivencia quinquenal fue de 18% y la decenal de 3.76%. Las necropsias demostraron que 95% de las mujeres fallecieron de carcinoma mamario y de ellas 75% tenía úlceras en la mama. Características biológicas del cáncer mamario: el adenocarcinoma escirroso típico comienza en el cuadrante superoexterno (45%) del seno izquierdo (60%) y se necesitan 30 duplicaciones a partir de la etapa unicelular, por un lapso de cinco a ocho años para que alcance un tamaño palpable (1 cm de diámetro).
La metástasis surgen cuando el tumor es de 0.5 cm de diámetro y el pronóstico recibe la influencia adversa del número de ganglios linfáticos axilares afectados. Con el agrandamiento mencionado la fibrosis acorta el ligamento de Cooper y hay la característica depresión u hoyuelo de la piel.
La diseminación sistémica es más común a pulmones (65%), hueso (56%) e hígado (56%).
La investigación diagnóstica se debe hacer en forma ordenada. En toda lesión sospechosa conviene realizar biopsia de aspiración y después por extirpación parcial (incisional), en dirección de los pliegues cutáneos (periareolar), o como un recurso cómodo en caso de posible resección segmentaria o mastectomía ulteriores. La clasificación por etapas puede hacerse antes del tratamiento definitivo e incluye una radiografía de tórax y pruebas de función hepática. No se requieren radiografías del esqueleto ni gammagrafías óseas cuando no existen síntomas específicos.
- Auto examen
Pasos a seguir
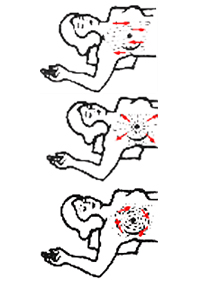 Recostada
Recostada- Ponga sus brazos en ambos costados
- Revise sus mamas buscando nódulos, retracciones, formas irregulares u otros cambios
- Repita el procedimiento con sus brazos encima de la cabeza.
- Ahora con sus manos sobre la cadera y los músculos torácicos tensionados.
- Finalmente, inclínese y observe sus mamas una vez más por cualquier cambio.
- Recuéstese de espaldas en una posición cómoda y coloque una almohada por debajo de su hombro izquierdo.
- Examine toda su mama izquierda con la mano derecha, siguiendo cada una de las figuras mostradas más abajo.
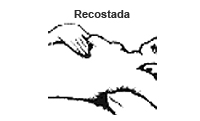 Coloque sus dedos de manera plana contra el tejido mamario, presionando de manera leve, mediana y firme haciendo círculos pequeños y más grandes.
Coloque sus dedos de manera plana contra el tejido mamario, presionando de manera leve, mediana y firme haciendo círculos pequeños y más grandes.- Ahora mueva la almohada a su hombro derecho y examine toda su mama derecha.
En la ducha
- Revise sus mamas y axilas para detectar algún nódulo o engrosamiento.
 Examine sus mamas en la ducha usando el mismo procedimiento que utilizó en el paso anterior.
Examine sus mamas en la ducha usando el mismo procedimiento que utilizó en el paso anterior.- Sus manos jabonosas se deslizarán más fácilmente sobre la piel mojada.
Notas
- Se recomienda no realizar este autoexamen en época premenstrual.
- Si usted percibe algún tipo de secreción del pezón durante estos procedimientos, o en cualquier momento, informe a su médico.