
- Centro Médico TeknonCentre Mèdic Quirónsalud Badalona
Pathologies or diseases of the thyroid can be treated medically and/or surgically.
Hyperthyroidism with small diffuse or nodular goiter, small uni or multinodular goiter, asymptomatic and benign, hypothyroidism presents a good response to medical treatment.
Other pathologies such as hyperthyroidism refractory to medical treatment, large and / or symptomatic goiter and thyroid cancer are surgical treatment.
Surgery plays a fundamental role in the treatment of thyroid diseases. The objective of the surgeon who should indicate thyroid surgery should be in cases of non-response to medical treatment, cases that present symptoms, are usually large goiters (dysphagia, airway obstruction, etc.) and thyroid cancer.
The degree of surgery to be performed (hemithyroidectomy, subtotal thyroidectomy, total thyroidectomy) must sometimes be determined during surgery.
- General
Anatomy
The thyroid gland weighs, on average, 15 g, and is composed of two lateral lobes that extend to the sides of the larynx to very close to the midline of the thyroid cartilage, and that are joined by an isthmus that pass in front of the trachea. In 80% of cases there is a pyramidal lobe that extends from the isthmus upwards and represents remains of the embryonic thyroglossal duct. For its upper part the thyroid receives blood from the external carotid and from the lower part of the thyrocervical trunk.
Physiology
The main function of the thyroid is to synthesize and secrete thyroid hormones. The increase of these raises the metabolic rate and vice versa. Calcitonin is produced by C cells and does not appear to have physiological intervention. Its therapeutic use is limited to the treatment of hypercalcemia and Paget's osteopathy, and as a tumor marker in medullary carcinoma.
Patient Evaluation
- Interrogation: The doctor should question the patient about signs of hyperfunction or insufficiency, pressure of the thyroid to adjacent structures, with the appearance of manifestations such as dysphagia, dysphonia, dyspnea or choking sensation. You also have to find out the presence or appearance of tumors, duration of it, their growth rate and the presence of pain. Contact with low doses of ionizing radiation is of enormous importance, as is the ingestion of goitrogen drugs. Is there a family history?
- Exploration: The doctor notices a visible mass or enlargement and deviation of the trachea. The seated patient is palpated from front to back to learn about the size and consistency of the gland and regional nodes.
- Autoimmunity indices: Antithyroglobulin and thyroid antimicrosomal antibodies are measured in serum. Thyroid scan. It is convenient to do a thyroid scan after administering Io Tc. The scintigraphic image shows that the nodule may be "hotter" than the rest of the gland, of equal thermal intensity or hypofunctional or cold. Many cancers appear as a simple, cold nodule.
- Ultrasound: Determine whether the lesion is cystic or solid. Many carcinomas are solid, while several cystic or mixed lesions are benign. Thyroid biopsy. Fine needle aspiration is useful in the diagnosis of thyroiditis and in differentiating between benign and malignant neoplasms
- Hyperthyroidism
Thyrotoxicosis is the primary excessive secretion of active thyroid hormone.
- Graves' disease. This is often thought of as a systemic autoimmune problem. Its clinical picture includes thyrotoxicosis, exophthalmia and pretibial myxedema. There is diffuse enlargement of the thyroid (smooth surface), showing hyperplasia in the microscopic section, with cylindrical epithelium and minimal colloid.
- Toxic multinodular goiter. It is usually overadded to long-standing non-toxic multinodular goiter. Nodules are composed of irregularly large cells and sparse colloid. It is an autonomic disorder, independent of the action of thyroid-stimulating hormone.
- Toxic adenoma. It is a follicular tumor, independent of thyroid-stimulating hormone.
Clinical manifestations
Thyrotoxicosis includes heat intolerance, increased sweating, thirst, and weight loss with intensification of appetite.
Excitability, restlessness, hyperkinesia, emotional instability, with insomnia, weakness of proximal muscles, tremor with the fingers in extension and abduction and hyperactivity of deep tendon reflexes.
The skin is hot, moist and congested, with fine hair that easily sheds, and in women there is a shortage or absence of menstruation.
The person may have diarrhea. In older patients it is possible to observe tachycardia with frequent atrial fibrillation and poor response to digitalis.
- Graves' disease. It affects rather young people, in proportion of one male for every six women. There is enlargement of the gland, which is smooth and with an audible murmur.
Eye signs range from minimal to intense:
a) Spasm of the upper eyelid, with retraction and greater interpalpebral opening.
b) External ophthalmoplejía.
c) Exoftalmía con proptosis.
d) Supra and infraorbital edema.
e) Congestion and edema, which are a sign of the intensity of the picture
- Toxic multinodular goiter. It usually arises after 50 years of age, with several palpable nodules. Exophthalmia is rare.
- Toxic adenoma. It affects people 30 to 50 years of age. There is a history of a slow-growing mass; Thyrotoxicosis is rare, unless the lesion is 3 cm in diameter.
- Diagnostic signs. There is an increase in the levels of T4, T3 or both hormones and also in the free thyroxine index (ITL). Graves' disease. For its diagnosis, diffuse goiter with exophthalmos and elevated thyroid function stand out. The uptake of radioactive iodine is 45 to 90%. The T3 suppression test is applicable; A decrease of 50% or less is a diagnostic sign of the problem.
- Toxic multinodular goiter and toxic adenoma. In these tables the uptake of radioactive iodine is 40 to 55%. The scan shows single or multiple "hot" areas that correspond to the palpable nodules
Treatament
- Antithyroid. Propylthiouracil (PTU) and methimazole. Antithyroid drugs have no action on the underlying disease. Measuring T4 and T3 levels is useful for assessing the reaction to treatment. Graves' disease is treated while waiting for natural remission to arise instead of the subject becoming euthyroid. Less than 40% of patients have significant lasting remissions. In people in whom thyrotoxicosis recurs or who do not comply with treatment, it is recommended to administer radioactive iodine or operate.
- Radioactive iodine. A dose of iodine is chosen, such that the subject receives 8 500 rad to the thyroid; 20% of people need a second dose. The treatment avoids the operation, with its rare complications, and reduces costs. Among the disadvantages are the long time needed to control the disease, the high incidence of permanent myxedema and the appearance of nodules. The risk of genetic abnormalities after radioactive iodine is administering is minimal. The second strategy is to administer high doses of radioactive iodine followed by gland replacement
Surgery
- Preparation. Antithyroids are given initially to control thyrotoxicosis and then, in the preoperative period, eight to 10 drops of iodized solution are added to decrease the vascularization of the gland. Some doctors prefer a five- to seven-day preparation with propranolol alone.
- Results. Mortality is less than 0.1%. With subtotal thyroidectomy, rapid correction is achieved in 95% of cases. Complications, with the frequency already noted, are: recurrent nerve palsy, 0 to 3%; hypoparathyroidism, 10 to 30% and recurrences in 2 to 12% of cases.
- Selection of treatment. Young, pregnant or breastfeeding people can receive antithyroid drugs and in case of failure thyroidectomy or radioactive iodine is used. Surgery is preferred in young people with severe disease and large goiters. Older people will receive radioactive iodine. One or the other treatment is used in toxic multinodular goiter. It is important to remove the toxic adenoma
- Hypothyroidism
This chart denotes the failure of the gland to maintain an adequate plasma level of thyroid hormones.
- Causes. It is known that 25% of cases depend on the removal of the gland by thyroidectomy or by administration of radioactive iodine to combat hyperthyroidism. Spontaneous myxedema sometimes results from aplasia or replacement of the gland by nonfunctional goiter, adenoma, or thyroiditis.
- Clinical manifestations. The picture may include cretinism, juvenile hypothyroidism and lymphocyte thyroiditis in adults, with an attack of 80% in women.
The course is progressive and insidious and includes tiredness, weight gain, fatigue and apathy. The skin is dry, thick and "bloated", the hair is dry and brittle.
There is enlargement of the tongue and the voice is hoarse; Cardiac output decreases, there is dilation of the heart and slowness of the pulse. Other signs are constipation, ascites, achlorhydria and pernicious anemia. - Diagnostic signs. They include anemia, bradycardia, flattening of T waves, and decreased levels of T4, T3, and free thyroxine index. There is an increase in TSH and cholesterol levels.
- Treatment. Replenishment, usually, with L-thyroxine. Severe cases react to small doses, so that the latter should initially be of the order of 50mg, to increase little by little and avoid imposing overloads on the myocardium
- Goiter
Goiter is a benign enlargement of the thyroid.
- Family goiter. It comprises an inherited enzyme defect, usually by an autosomal recessive mechanism.
- Endemic goiter. It is a regional environmental form in which there is iodine deficiency and the subject ingests biociógenos. In these cases, prophylactic iodization of domestic salt should be carried out.
- Sporadic goiter. This is a diagnosis of exclusion.
Pathology
Diffuse enlargement of the gland is noticed, which has a smooth or strongly nodular appearance. Early hyperplasia is reversible. Involution is identified, with large colloid-filled follicles interspersed with normal tissues. Clinical manifestations. Goiter appears in endemic regions without differentiating in its attack on one sex or another, although sometimes a ratio of eight women to one affected male is noticed. It is rather asymptomatic, but may present dysphagia, tracheal compression, with respiratory dysfunction, particularly in case of substernal extension. If bleeding occurs, there may be sudden pain and rapid expansion. The disorder rarely causes hypothyroidism, but thyrotoxicosis occurs in a large percentage of cases with a long-standing history.
Diagnostic data
Thyroid function test results are usually normal. Chest and neck x-rays should be obtained to identify the extent of the goiter around the trachea and behind the breastbone.
Treatment
In diffuse goiter, the familial type improves with thyroxine. Drug-induced goiter forces to interrupt contact with the harmful substance; If this is not possible, thyroxine is administered. Surgical indications include airway obstruction and unsightly appearance. Whenever an important segment of the thyroid with goiter is removed, thyroid hormones should be administered as a form of replacement.
- Lonely Nodules
In the United States it has been reported that 4 to 6% of the population has palpable thyroid nodules; 50 people per million have thyroid cancer and six per million die of this neoplasm.
Groups at high risk of cancer
People who have received radiation to the head and neck are at high risk: there is a direct increase in incidence in benign and malignant nodules at doses of 1,500 rad, but only after latency of 25 years or more.
The original treatment was applied to combat enlargement of the thymus, tonsils and adenoids, or against acne and hemangiomas. It is usually a papillary form and often multicentric. There is a family history of medullary carcinoma and there is an autosomal dominant trait.
Diagnostic assessment
Select for surgery nodules with risk of being malignant. Investigate the following data in the patient:
- External radiation.
- Onset time (recent or growing).
- Age and sex (any nodule in children or adolescents or new nodule in males > 40 or females> 50, likely to be malignant, few nodules in males are benign).
- Hoarse voice (recurrent nerve invasion).
- Dyspnea or dysphagia (compression).
Physical exam
- Solitary (unless there is a history of radiation), firm or hard, fixed. Lymph node growth, think malignant condition.
- Fine needle aspiration for cytology. Nodules are classified into malignant (surgery), follicular cell sheets indicating follicular adenoma or carcinoma that can only be differentiated with histology (surgery), colloid nodule (observe, unless it causes symptoms), or non-diagnosis.
- Gammagram with isotopes or ultrasound. They are rarely indicated.
- Accurate computer tomography (CT) and magnetic resonance imaging (MRI) are reserved for large, difficult lesions
- Benign tumors
Adenomas are embryonic, fetal, follicular or microfollicular. It is known that 60% of surgical pieces with a single nodule contain a benign type of neoplasm.
Clinical manifestations. Tumors are slow-growing masses that are sometimes "cold," "hot," or barely "warm".
- Malignant Tumors
These are papillary, follicular, medullary and anaplastic cancers, as well as lymphoma and metastases from other cancers.
Carcinoma papilar
It has been observed that of all cancers of this type, 66% correspond to the thyroid. The frequency of attack peaks in the third and fourth decades. It is more harmful in the elderly subject. The sex ratio is three females to one male. Slow growth, intraglandular spread (40% invades the contralateral lobe) and to regional lymph nodes, central and upper mediastinal compartment, then jugular and finally lungs. In nuclear cytology, size variation, nucleoli and "segmented nuclei".
- Clinical manifestations. The nodules are asymptomatic and there are calcium stretch marks on thyroid x-rays. treatment. In lesions <1 cm in diameter without invasion through the thyroid capsule in young people, lobectomy and thyroid hormone are sufficient in the postoperative period to suppress TSH. If the lesion > 1 cm in diameter, total thyroidectomy or almost. If a tumor is found in a lymph node in the lateral triangle, a modified radical neck dissection is indicated. Prophylactic neck dissection should not be done. With total removal of the thyroid, papillary metastases will pick up and can be treated with radioactive iodine. Suppressive doses of thyroid hormone are given for life.
- Prognosis. It is excellent in young people, but the picture worsens in people over 50 years of age. Overall, 10 to 12% of patients die from the disorder. Complex schemes are presented to make the forecast.
Follicular carcinoma
This type comprises 18% of thyroid cancers, with peak incidence in the fifth decade of life. The frequency by sex is three females for every male.
The neoplasm shows clear, more unicentric encapsulation. The follicles have precise histological features, but the cells may be crowded and malignant, with capsular and vascular invasion. There is hematogenous spread to bones, lungs or liver in early evolution.
- Clinical manifestations. Recent change in old date goiter. Usually there is only one solitary nodule, but in the late phase pain and adhesions arise. Metastases usually concentrate iodine.
- Treatment and prognosis. There is controversy regarding the magnitude of the resection, some surgeons are inclined to the elimination of the lobe and isthmus in the face of minimal disease, while others prefer subtotal or total thyroidectomy to facilitate the scintigraphy of the body and the treatment of metastases by means of radioactive iodine. This form is more aggressive than papillary and decadal survival is 72 percent.
Other treatments for differentiated cancers
- Thyroxine. After surgery, sufficient doses of L-thyroxine are administered to suppress circulating thyroid stimulating hormone levels.
- Administration of radioactive iodine. A whole body scan with radioactive iodine is done and the normal residual thyroid tissue in the neck is removed; also to treat any distant metastases, identified with I. External-beam radiation is applied in case of invasion of the trachea or esophagus. Chemotherapy. Doxorubicin is used on highly metastatic lesions that no longer concentrate iodine.
Hürhle cell tumors
Tumors of this type are formed of layers of cells with eosinophilic cytoplasm; Some are obviously malignant, with lymph node invasion and spread, while others have a benign appearance. These tumors do not concentrate iodine. It is undertaken with a history of radiation, in large lesions, in cases of capsular invasion and when accompanied by differentiated carcinoma. Lobectomy is done to treat small masses with benign histologic imaging.
Medullary carcinoma
C cells produce calcitonin and come from the neural crest. Carcinoma can cause the so-called APUD syndrome. It appears in the posteroexternal portion of the gland.
The size of medullary carcinoma can vary from microscopic dimensions to 10 cm in diameter. The norm in family cases is bilateral attack. Clusters of cells separated by area of collagen and amyloid are observed; They can be polyhedral and simulate carcinoid or spindle cells. The neoplasm spreads to regional nodes in the neck and upper portion of the mediastinum and from there to distal areas.
- Clinical picture. Medullary carcinoma comprises 3.5 to 11.9% of thyroid cancers. On average, the familial form is manifested between 20 and 25 years (multiple endocrine neoplasia type IIA in older cases of type IIB in minors), by an autosomal dominant mechanism. Nodules can be isolated or multiple and at the time of diagnosis there are already lymph node metastases in 15 to 20% of cases. Diarrhea is common, with episodic hyperemia and 2 to 4% of patients have Cushing's syndrome due to ectopic ACTH production. There is a relationship between hypercalcemia and pheochromocytomas.
- Familial medullary carcinoma syndrome. The NEM-IIA (multiple endocrine neoplasia) variety includes multicentric medullary carcinoma or C-cell hyperplasia, pheochromocytomas or medullary hyperplasia, and hyperparathyroidism. The group of MEN-IIB neoplasms includes medullary carcinoma (particularly virulent), pheochromocytomas and mucosal neuromas of the lips, tongue or conjunctiva, intestinal ganglioneuromas, typical facies and marfanoid complexion. Adrenal medullary hyperplasia or pheochromocytomas are multicentric in 70% of cases. The latter can be malignant and metastases are more frequent when the primary tumor is outside the adrenals.
- Diagnosis. Among the laboratory studies, a higher serum level of calcitonin is observed by means of radioimmunoassay and thyroid mass is a diagnostic data. It is important to study family members to detect injuries early. There may be an increase in carcinoembryonic antigen. The reappearance of serum increases of this antigen denotes tumor recurrence. In the preoperative period, catecholamines and serum calcium should be studied.
- Treatment. In these cases, total thyroidectomy is needed, due to the multicentric nature of the lesion. Up to 50% of patients show lymph node metastases from neoplasia. Neck dissection will be done if there is clinical involvement of the lymph nodes. Thallium scintigraphy allows metastases to be located. Decreasing tumor mass by surgery lessens the effects of APUD. Chemotherapy will be attempted in cases of progressive metastases. First of all, pheochromocytomas must be operated; The total removal of both adrenals is the most common operation, given the multicentric nature of the neoplasm. The parathyroid lesion comprises major cell hyperplasia.
- Prognosis. Survival is 80% at five years and 57% at 10 years.
Carcinoma anaplásico
This type of carcinoma comprises 10% of thyroid cancers. It can arise by transformation of a differentiated tumor. The attack ratio between males and females is 3:1. Half of the cases appear between 60 and 79 years and the average age in this neoplasm is 66 years.
Neoplasm without a frank capsule invades neighboring structures. The histological picture is that of cellular structures ranging from spindle cells to giant multinucleates; Mitosis is abundant. The initial picture includes painful enlargement of the thyroid, sometimes with fixation of the gland; The effects of pressure are common. It sends metastases to the lung. It is rarely resectable. The diagnosis is made by needle biopsy and then complementary treatment is started. Up to 75% of patients die within one year of diagnosis.
Lymphoma and sarcoma
The thyroid is a rare site for the occurrence of primary lymphoma. Some limited technique is needed to confirm the histological diagnosis and then undertake radiotherapy, chemotherapy or both therapeutic modalities.
Metastatic carcinoma
2% to 4% of patients who die of cancer have thyroid metastases. The primary ones that most frequently produce them are lung cancer and hypernephroma.
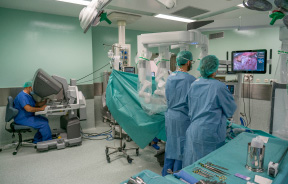
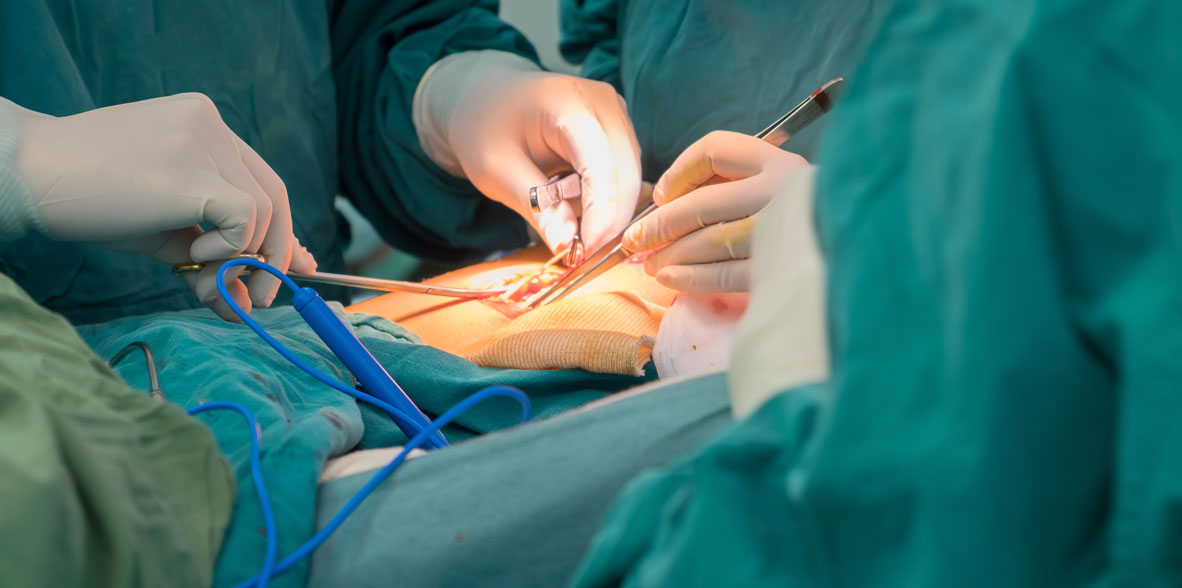
Thyroid surgery
This gland is operated in order to diagnose some mass inside, remove benign and malignant tumors, treat thyrotoxicosis or relieve pressure symptoms attributable to it.
- Operative technique. First, endotracheal anesthesia is performed and the patient is placed with the neck in extension. The surgeon makes an equilateral incision in a fold of skin, as a "low collar." A lower flap is raised and carried to the sternal notch.
In the midline the cervical aponeurosis is sectioned. The sternothyroid and sternohyoid muscles are separated or, if the gland is large, sectioned. The lobe turns inward and the middle thyroid veins are controlled and sectioned. The surgeon penetrates the cricothyroid space. It also identifies and preserves the outer branch of the superior laryngeal nerve that goes to the inferior constrictor of the pharynx and cricothyroid muscles.
The vessels of the upper pole are ligated separately, near the lobe, and sectioned. The lobe retracts inward and the branches of the inferior thyroid artery, near the capsule, are ligated and sectioned to preserve circulation to the parathyroids.
The recurrent laryngeal nerve is gently discovered. In the operation for Graves' disease, 2 to 4 grams of posterior thyroid tissue are left and folded against the trachea or the lobe is removed in its entirety. It is important for the surgeon to identify and preserve the parathyroids and their blood supply.
The isthmus separates from the anterior portion of the trachea, leaving no tissue remnants. The incision is closed in layers. Intrathoracic goiter usually represents an extension of cervical thyroid tissue inside the chest and is removed through an incision in the neck. Sometimes the transsternal approach is needed. - Complications. Thyroid storm. It occurs in subjects with persistent thyrotoxicosis who have not been treated or who have been treated incompletely. Manifestations may arise in the operating room or recovery room. The picture includes hyperthermia, sweating, tachycardia, nausea, vomiting and pain. Tremor and restlessness may progress to delirium or coma. Treatment includes large doses of sodium iodide or potassium intravenously, 100 mg cortisol, oxygen and large doses of glucose, "proportionate" (balanced) hydroelectrolyte solutions, a hypothermia blanket and propranolol or other beta-blockers. Mortality is approaching 10 percent.
- Hemorrhage from the incision. This complication arises within the first hours of the postoperative period. It causes respiratory dysfunction because small amounts of blood in the deep space very close to the trachea obstruct the airway; This complication arises in 0.3 to 1% of cases. Treatment is urgent. The wound must be opened, the clot evacuated, pressure applied, the patient must be taken to the operating room and the hemorrhagic vessel must be inhibited.
- Recurrent laryngeal nerve injury. Complication that appears in 1 to 3% of thyroid interventions. They can be unilateral or bilateral, temporary (three to twelve months) or permanent. In case of paralysis of the abductor muscles of the vocal cords in the larynx, they assume a medial position. The voice is dull and hoarse. Bilateral paralysis of the cords can lead to airway dysfunction.
- Hypoparathyroidism. The frequency of this disorder is 0.6 to 2.8%. It is even more common (9%) during cancer treatment, particularly in secondary procedures. It is rarely due to removal of all glands. It is more likely to depend on irrigation disturbance. The risk is minimized by ligation of the vessels in the thyroid capsule. The devascularized gland can be crumbled and implanted in pockets in the sternocleidomastoid. The picture manifests a few days after the operation and includes perioral insensitivity, tingling of the fingertips, anguish, Chvostek's sign initially, followed by trousseau and carpopedal spasm. The picture can evolve into tetany. There is hypocalcemia and hyperphosphatemia. The disorder may be transient (days) or permanent. Treatment includes 10 ml of 10% calcium gluconate intravenously in slow direct drip and then venoclysis in which two or three vials of calcium gluconate are introduced every eight hours. Oral administration of calcium can be started to provide 1.5 to 2 grams per day. In permanent hypoparathyroidism, vitamin D (Rocaltrol, 0.25 to 0.5 g/day in addition to calcium) will be required. Measure calcium and high phosphorus in hypoparathyroidism. Low in "hungry bone syndrome"
If you need thyroid surgery, it's important to know which one to expect. The following are some of the most frequently asked questions as possible.
How long will I be hospitalized?
According to the surgery performed and the evolution of the postoperative period but generally between 24 and 72 hours after the intervention. In selected cases, outpatient surgery may be offered.
What type of anesthesia?
General anesthesia
Do I have a scar?
All surgery causes yes to mark with a scar, and how the scars patients are dependent on the individual.
However, there are some techniques that surgeons use to minimize scarring. These techniques include: a smaller incision size, careful incision placement, and hypoallergic suture material (prevent inflammation).
As a rule, it is unusual for adults to have a tender scar after six months.
Do I have pain after the operation?
All operations involve some pain and discomfort. Our goal is to minimize this discomfort. Although you should be able to eat and drink normally, the main complaint is pain with swallowing.
When will I know the results of the surgery?
During the operation, your surgeon will consult with the pathologist who will provide a preliminary diagnosis. However, the final report of the pathology requires careful study of the surgical specimen. Therefore, the final report is not usually available until about a week after the operation.
Do I have physical restrictions after my surgery?
Swimming is the only main restriction. In general, your activity level depends on the amount of discomfort you experience. Most patients can return to work within the first two weeks, and you can drive as soon as your head can be turned comfortably (this limitation is for driver safety). Post-surgery visits with your surgeon will expand the information of your incorporation into the normality of the daily routine.
What are the complications unique to thyroid surgery?
In about 1 in 250 thyroid operations, the nerves that control the voice are affected by thyroid surgery. When this occurs, the main difficulties are voice projection and production of high-pitched and/or loud sounds or when trying to shout.
It is usually described as hoarse and/or aphony. Generally, voice changes are temporary, so the voice will return to normal within a few weeks; Permanent change is rare.
In about 1 in 300 thyroid operations, the parathyroid glands will not function as a result of surgery. These are four glands that are located near the thyroid.
Since the parathyroid glands control calcium levels, their dysfunction usually results in a low level of calcium. Therefore, some patients require calcium supplementation on a temporary basis.
If the parathyroids do not function properly, calcium or vitamin D may be needed on a permanent basis.