López Gil Francisco José
Who gets skin cancer and why?
Skin cancer is caused by exposure to ultraviolet rays either directly from the sun or from tanning beds.
Other contributing factors are:
- If you are fair-skinned and therefore burn easily
- If you work outdoors or do sports in sunny climates
- If members of your family have had skin cancer or have many nevi (moles or freckles)
- If you had serious sunburn as a child
- If you have either a lot of nevi (100 or more) and/or they are larger than average (bigger than 0.5cm) and/or they have an irregular shape
- If you have had radiotherapy
How can I prevent skin cancer?
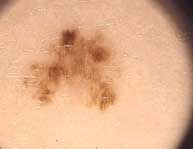
1. Go immediately to a dermatologist if you have a skin lesion that bleeds, itches, doesn't heal or is growing rapidly.
2. Have a skin check-up once a year with a dermatologist and learn to do a regular self examination of existing moles, birthmarks, brown spots or beauty marks checking for the following symptoms:
A. If It is irregular in outline
B. If It changes colour (of there is a variation of colour in the same lesion)
C. If It has a diameter greater than 6mm
D. If It changes in texture or thickness
 The FotoFinder is an imaging system that allows the dermatologist to accurately identify the potentially dangerous skin lesions. It takes a photographic "map" of the skin ensuring a much more precise system of skin cancer control throughout the whole of a person's life.
The FotoFinder is an imaging system that allows the dermatologist to accurately identify the potentially dangerous skin lesions. It takes a photographic "map" of the skin ensuring a much more precise system of skin cancer control throughout the whole of a person's life.
Safe tanning advice
1. If you can see sunlight seek the shade. A good guide is that if the shade you project is smaller than you, you are more likely to burn. The sun's rays are more frequent, and the possibility of developing sunburn is greater, between the hours of 10am and 4pm.
2. Regularly apply sun protection of no less than SPF15 when exposed to the sun and undertaking any kind of outdoor activity. Apply the sunscreen 20 or 30 minutes before going out into the sun so that it has time to be absorbed. Also ensure that the zones that we easily forget about are covered for example: - the ears, lips, around the eyes, neck, exposed parts of the head, hands and feet.
3. Reapply the sun protection every two hours or whenever you are outside even if it's cloudy. Obviously it's easier to burn on a hot day because the heat increases the effects of the UV rays but you can also burn on cloudy days. Also reapply after swimming or if you are undertaking a sport where you are sweating as these types of activities remove the sun protection.
4. Try to always wear protective clothing like a big hat, long trousers and long-sleeved tops. The thicker and darker the clothing the better protection is will give you. Be careful as water makes the material become more translucent.
5. Be careful if you are taking medications that can induce photosensitivity. Always check with your doctor or pharmacist if it seems that the medication is capable of producing extreme reactions to sunlight characterised by a rash, redness or swelling.
What are the most common types of skin cancer?
- Basal Cell Carcinoma is the most common form of skin cancer. It is rarely life-threatening, grows slowly and almost never spreads.
- Squamous Cell Carcinoma is the second most frequent and usually occurs on the areas most exposed to the sun: - the lips, ears, back of the hands etc. In contrast to the previous kind of skin cancer, this kind can invade lymphatic ganglions and internal organs and is therefore dangerous.
- Melanoma is the less frequent form of skin cancer but is the most dangerous. However, if Melanoma is recognised and treated early it is almost always curable.
Treatment of skin cancer
Basal Cell Carcinoma
The Basal Cell Carcinoma is a malignant tumour that only affects the site area and is not invasive. The most common and effective form of treatment is surgery.
Squamous Cell Carcinoma
The Squamous Cell Carcinoma is much more aggressive than Basal Cell Carcinoma so surgical removal is the preferred form of treatment. Sometimes a course of radiotherapy is also necessary.
Malignant Melanoma
Malignant Melanoma is always treated surgically. The main prognostic factor in this disease is the depth measured in millimetres (Breslow) and this data determines the width and depth of the surgery. Similarly if the depth exceeds 1mm then it is necessary to investigate the status of lymph nodes close to the skin lesion (Sentinel Node Biopsy) to determine if the tumour has spread to other parts of the body.
| Morning | Afternoon | |
|---|---|---|
| Monday | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Tuesday | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Wednesday | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Thursday | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Friday | 09.30 - 13.30 h | 15.30 - 19.00 h |















