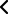FACULTATIVO ESPECIALISTA CIR. ORTOPÉDICA Y TRAUMATOLOGÍATraumatología y Cirugía OrtopédicaCentro Médico Teknonen/health-centers/centro-medico-teknon
FACULTATIVO ESPECIALISTA CIR. ORTOPÉDICA Y TRAUMATOLOGÍATraumatología y Cirugía OrtopédicaCentro Médico Teknonen/health-centers/centro-medico-teknon
Disk replacement surgery
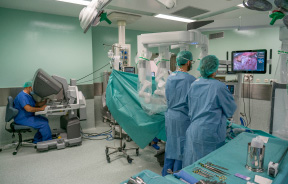
The goal of disk replacement is to replace a damaged or degenerated disk in the lumbar spine with an interbody cage or a disk prothesis. Disk replacement surgery is done with only a small incision on the patient’s belly (abdomen). By approaching the lumbar spine through the front (anterior approach), dissection of muscles, bone structures and nerves are avoided. All these major structures are on the way when approaching the lumbar spine through the back (posterior approach). Hence, with disk replacement surgery, the risk of damaging nerves and muscles is low.

Layout (left image) of the anterior approach to a lumbar spine disc. A large interbody
cage can be placed in the discwith the anterior approach (right image).
The advantages of disk replacement surgery is that it allows an excellent exposure of the lumbar spine from the front (anterior approach). This allows introducing large interbody cages and artificial discs with a much larger surface area compared to those introduced through the back of the patient (posterior approach).

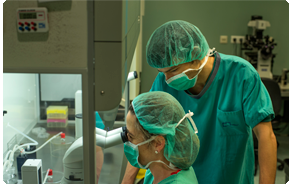
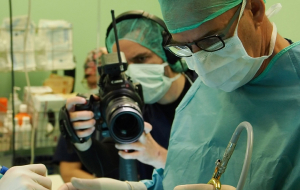
Dr. Morgentern (back left) performing the anterior retroperitoneal approach.
Disk replacement is a minimally invasive spine surgery, as all the structures contained in the peritoneal sac (intestines, organs, etc.) are bypassed bluntly, no important tissues are cut nor resected. Therefore, the patient usually shows a speedy and complete post-operative recovery . The patient resumes walking the same day of surgery and can go home (hospital discharge) usually just 2 days after the surgery.

Tiger Woods by Keith Allison
One of the most popular cases of a successful disk replacement surgery performed is the case of the golfer Tiger Woods, champion of the Augusta Masters 2019. He returned to playing as pro-golfer successfully after having undergone an operation on the lumbar spine through an anterior route in the USA.
Dr. Morgenstern has been trained in Germany to perform disk replacement spine surgery. This surgery complements the endoscopic and percutaneous surgical techniques and helps us avoiding other invasive surgeries of the lumbar spine.
Who is eligible for for disk replacement surgery (ALIF)
Degenerative disk disease (DDD) is an illness describing an interbody disk (located between two vertebral bodies) that has progressively lost its original height due to the aging process and overloading. A degenerated disk often causes intensive pain in the lower back and buttock area. A complete collapse of the disk height can also lead to foraminal stenosis with an impingement of the exiting nerve roots, causing sciatic pain that radiates to one leg. Hence, disk replacement surgery is indicated for acute and chronic low back pain with or without radiating leg pain.

This picture shows an intra-operative X-ray image of an
interbody cage placed at level L5/S1. Note the screws
attaching the cage to the upper and lower endplates o
f the adjacent vertebrae.
Disk replacement surgery replaces the degenerated disk with an interbody cage and restore the disk’s height. Disk replacement surgery is a minimally invasive surgery with a speedy recovery. The patient usually walks in his room during the same day after disk replacement surgery and hospital discharge is usually within two days after surgery. Low back pain and radiating leg pain usually are relieved immediately or in less than 24 hours after surgery.

Final X-ray control of two interbody cages placed anteriorly at levels L4-L5 and L5-S1
attached with three screws to the upper and lower vertebral endplates, respectively.
Caso Clínico Abordage anterior (ALIF) y lateral-oblícuo (OLIF)
Video showing a case of an anterior and oblique-lateral approach of
a 53 years-old patient that was only able to walk with the help of a
stick because of strong low back pain. The patient was able to start
walking without pain 12 hours after surgery and hospital discharge in
less than 48 hours after surgery.
Clinical Case of an anterior lumbar interbody fusion (ALIF)