López Gil Francisco José
What is psoriasis?
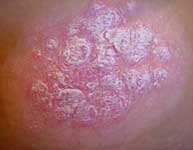
Psoriasis is a chronic autoimmune disease that causes outbreaks of usually red scaly patches on areas such as the elbows, knees and scalp although it can also affect other areas such as the nails and joints.
It is never contagious and therefore no precautions are necessary for somebody caring for a person with psoriasis.
When and why does it appear?
It can start at any age but most commonly between 15 and 35 years of age. The development of the disease is very unpredictable; often reoccurring throughout the life of the patient but is always benign.
The outbreaks can last from a few weeks up to several months. Usually the plaques or patches of affected skin will often improve if not totally disappear between episodes and sometimes the person may look completely better. These remissions can happen spontaneously.
What are the current treatments?
Topical treatments
The most common way of treating psoriasis is the use of creams containing corticosteroids and derivatives of vitamin D but the results are generally unsatisfactory.
One of our best allies in fighting psoriasis is the sun. However, It is important to remember to keep the skin well hydrated both during and after your time in the sun for it to be effective.
Oral treatments
- Acitretin (Neotigason®): This regulates the growth and differentiation of the Keratin cells and it has anti-inflammatory properties. It is particularly effective for pustular psoriasis, palmoplantar psoriasis and thick plaque psoriasis. This treatment is especially effective if combined with either natural or artificial sunlight. Acitretin must not be taken during pregnancy as it can damage an unborn child and cause birth defects. Other general side effects include:- disturbed liver function (so the levels of liver enzymes and blood lipids will be closely monitored on this treatment) and also cutaneous effects:- dry eyes, dry lips and mouth, hair loss. It is also possible to experience muscular and joint pain if taking a high dosage.
- Methotrexate: This is a successful and popular medicine when treating severe psoriatic arthritis and other forms of psoriasis especially rapid onset or less extensive forms of psoriasis which have proved resistant to other forms of therapy. Also it is a good option in those cases where the patient is suffering psychologically with the disease. Basically it has a strong anti inflammatory effect and it is administered once a week for up to 12 weeks either orally or intramuscularly. This treatment should not be given to anyone who has chronic renal failure, or to people with severe liver disease or alcoholics, as it can also damage the liver. There is also a possibility in longer term medication that the bone marrow can be affected. Common side effects are: nausea, loss of appetite, fatigue and headaches in the 24 hours after having the medication.
- Ciclosporin: This is an anti-inflammatory and immune suppressant drug (it lowers the defences) used to treat chronic plaque psoriasis and substantially improves nails and arthritis when used on a long-term basis. The most frequent and debilitating side effect is kidney damage which depends above all on the quantity of the daily dosage and If this exceeds 3mg per kilo of body weight per day. Fortunately and thanks to early detection this kidney damage is completely reversible after the treatment is discontinued. It can also possibly cause high blood pressure which will then return to normal once the treatment is stopped. Other side effects are hipertrichosis (increased body hair), trembling and fatigue.
- PUVA: This is photo chemotherapy and is a combination treatment consisting of Psoralens (P) and then exposing the skin to UVA. The patient is given a photosensitiser in either tablet form or suppository (8-methoxypsoralen, trimethoxypsoralen) and two hours later is given a controlled dosage of UVA treatment according to the patient's skin and individual requirements. It is recommended to have these sessions as late as possible in the day otherwise the patient needs to protect their eyes with sunglasses for the following 8 hours.
Biological treatments for psoriasis
This kind of therapy is used in adult patients with moderate or severe psoriasis when the patient has no contraindications, does not tolerate or does not respond to other drugs used for the treatment of this disease. (Photo chemotherapy, methotrexate, acitretin and/or ciclosporin).
Due to the way it works regular medical checks are essential which can include a blood test, a chest x-ray and a Mantoux skin test.
The biological drugs are self-administered on a weekly or monthly basis using a subcutaneous injection pen depending on the type of medication used.
The treatment (whether it is topical, systemic or biological) should be individually personalized in each case bearing in mind the age, sex, habits, past medical history, the type of psoriasis and the previous treatments given. Taking into account all of these factors the dermatologist, along with the patient, will choose the most appropriate form of treatment.
- Etanercept (Enbrel®): This has a therapeutic effect on the skin lesions caused by the psoriasis and also an anti-inflammatory effect on the joints (psoriatic arthritis). It comes in syringes that the patient self administers subcutaneously once or twice a week for periods of up to 6 months.
The most common adverse effects are headaches and the local inflammatory effects of the injections.
Etanercept is contraindicated in patients with a history of serious infections, advanced heart failure, demyelinating disease or cancer.
| Matí | Tarda | |
|---|---|---|
| Dilluns | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Dimarts | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Dimecres | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Dijous | 09.30 - 13.30 h | 15.30 - 19.00 h |
| Divendres | 09.30 - 13.30 h | 15.30 - 19.00 h |















